Some claim the early television experiments in 1955 as the origin of TeleHealth, which means TeleHealth is more than half a century old. The adoption of TeleHealth has had multiple challenges including, but not limited to reimbursements, affordability and experience gaps.
However, of late, the stars are aligning for TeleHealth adoption to take off. According to BCC research, the global telemedicine market is expected to grow to 27.3 billion by 2016. According to the AHA (American Hospital Association) report, 42% of US acute care hospitals have TeleHealth capabilities. While healthcare reforms have given the adoption a significant boost, there are more trends that are fueling the adoption. We look at 10 such trends. On a broad level, these can be classified into three major categories:
- Policies and New Business Models
- Technology and Affordability
- Experience and Efficiencies
Here are 10 trends that are influencing the adoption curve: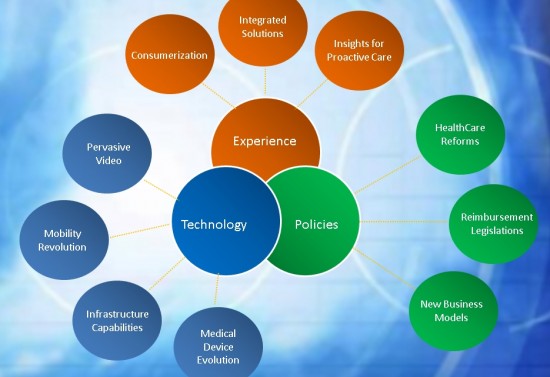
1. Paradigm shift generated by the Healthcare Reforms
The US healthcare reforms have created a fundamental paradigm shift in focusing efforts on driving wellness and preventive care as compared to episodic care. The longer term relationship between the patients and provider has put patient engagement and care coordination at the center. This need has created a renewed interest in
TeleHealth as it can provide not only a convenient and cost effective way to interact, but also drive experience and efficiencies for the patients and providers by providing better collaboration capabilities from anywhere.
2. Policy Changes and Legislation for Reimbursements
In the early days, as we talked to customers, we have constantly had the wow moment driven by technology and experience of our solutions, but when it comes to the reimbursement topic, the conversation would come to a full stop. Today, with the new long term wellness focus as opposed to episodic care, cost avoidance models, Reimbursement is no more a definite full stop. States have been catching up recently on its policies to support telemedicine. About 40 states allow Medicaid to pay for telemedicine visits and about 20 states have required private payers in the state to pay for telemedicine.
3. New business models
While the transition from pay-for-service to value based model happens, new innovative business models are emerging that drives TeleHealth towards a sustainable business. For example, a fixed flat fee based anywhere consults, corporate clinic models, cost avoidance strategies, wellness have created a renewed interest in TeleHealth
4. Pervasive Video
In the past, the promise of TeleHealth use to be ‘don’t travel 200 miles to see your specialist, you can get the services at your rural clinic”, which might still be few miles away. With pervasive video, the patient don’t have to even leave their homes and can have consults from their choice of devices which could be a mobile phone, a tablet, a laptop, video phones or any other specialized devices. The cost of video has also significantly come down lately and has improved the affordability of TeleHealth programs. Leveraging software based video solutions in addition to hardware has expanded reach not just within the enterprise boundaries, but also outside to create a borderless collaboration experience between providers. The rise of WebRTC and other video standards have increased interoperability and will further expand the adoption.
5. Evolution of the Medical devices
In the early days of TeleHealth, if you look at a TeleHealth examination room table, it can be pretty scary for a patient. There can be way too many cables and too many bulky boxes to which the devices are connected. The complexity and the cost of medical devices has been a hindrance to adoption.
The cost and complexity of medical devices have also significantly improved lately. The evolution to smaller, cost effective, consumer focused devices with wireless connectivity has improved user experience and has expanded the range of users. Internet of things enabled device connectivity and the ability to automatically obtain data from sensors can be used to track vital signs and other activities to understand early signs.
6. The Mobility Revolution
Mobility has not only changed how patients use the system, but also has influenced how providers are able to provide better and faster care. The initial definition of mobility in TeleHealth was the mobile carts. But with the advent of the smart phones and the tablets and increased focus on patient engagement, the access to the system has expanded significantly. The BYOD enabled choices for patients and providers and the mobile apps that enable video collaboration have helped patients to be more engaged in their care and in turn have further expanded access and demand for even more value added services.
7. Infrastructure and Delivery Models
In the past, the infrastructure cost and complexity of starting a TeleHealth project has been a major concern. Even after the initial deployment, the availability of network bandwidth has been equally challenging and need for dedicated lines have limited the RoI for operational economics.
Today, with the advent of Cloud and as a service models, not only are we able to get projects off the ground faster, but also are able to provide agility in introducing new capabilities. Adaptive network infrastructure and enhanced encoding has resulted in better usage of network and system resources.
8. Consumerization of Patients
The transition of patient to consumers has created significant pressure on providers to provide services that are consumer focused. The consumers expect the same level of experience that they have been used to in other segments such as banking and retail. For example, mobile apps is no more a choice, it is a necessity. While there might not be a payment model for some of these services, the absence of such services results in consumers moving away from current providers to competitors.
Patients have been demanding choice and increased experience and convenience and are critical to maintaining patient base. This is resulting in the use of TeleHealth to provide more patient engagement services to patients.
9. Integrated solutions
One of the key challenges for providers have been that TeleHealth solutions reside as silos and they had to use multiple systems to manage the day to day patient care and to access TeleHealth. This affects the usability, experience and has been a major reason for lack of interest in TeleHealth by providers.
Today, we are seeing more integrated solutions that incorporate TeleHealth within the EMR systems and helps avoid disruption of clinical workflows. In addition, the ability of systems to interface with backend systems and the ability to exchange data is enhancing provider experience and enabling continuity of care.
10. Increased Insights for Proactive Care
As more and more devices are connected and have the ability to generate more data, TeleHealth has become a value added system to provide better data capture opportunities for patient care. By leveraging the power of analytics and other technologies, valuable insights can be generated, and this enables proactive wellness and better quality of life for patients. This not only helps identify early signs and enable intervention, but also helps predict and plan better population health management.
These trends have aligned to accelerate the adoption of TeleHealth.
The 19th ATA conference is underway at Baltimore from 17th to 20th, May, 2014. Visit the Cisco booth at the conference to understand how Cisco’s TeleHealth technologies are enabling adoption of TeleHealth.





